Silakan login untuk mengakses laman berikut
THE FUTURE OF PRIMARY CARE MEDICINE
 First, every reader please vote for Delaware’s own Elena Delle Donne for the Naismith Women’s College Player of the Year Trophy. Vote by texting to **VOTE (**8683) beginning March 25. Naismith Trophy sponsor AT&T has opened the voting to customers of other wireless carriers. Congratulations, Miss Delle Donne. Thanks for your refreshing and energizing story of strength of character and success at your chosen sport. We pray for your continued success, your health, your team and your family.
First, every reader please vote for Delaware’s own Elena Delle Donne for the Naismith Women’s College Player of the Year Trophy. Vote by texting to **VOTE (**8683) beginning March 25. Naismith Trophy sponsor AT&T has opened the voting to customers of other wireless carriers. Congratulations, Miss Delle Donne. Thanks for your refreshing and energizing story of strength of character and success at your chosen sport. We pray for your continued success, your health, your team and your family.
Primary care medicine in Delaware
Primary care medicine in Delaware today is largely a cottage industry of small private practices. But things are starting to change. The hospitals have hired some primary care doctors and set up satellite offices throughout their service areas. The federally qualified health centers provide some primary care. In the region and nationally, we see physician practices merging to form large practices. Most practices have purchased computerized electronic medical records. We are all having trouble recruiting new primary care doctors.
The future of primary care in Delaware and in our region
They say that the primary care provider will be at the center of the medical delivery system of the future. The primary care physician is trained to evaluate a patient’s overall health status and co-morbidities – something a heavily specialized health care delivery system fails to do effectively. He serves as the patient’s principal guide through the health care system maze. Primary care is on the frontline, diagnosing new illnesses and managing chronic ones.
But what will this look like? How do we change the way physicians are organized in practice and how they are paid? How can we get the investments in infrastructure required to deliver comprehensive primary care so that the patient does not have to resort to expensive emergency rooms, hospitals and specialty procedures when they are not necessary?
Here are some changes we are seeing already or may see soon.
1. The primary care provider may not be your doctor. He may be a nurse practitioner, a physician assistant, a pharmacist or a health coach. He may be somebody from your health insurance company. Although most agree that your physician should be the manager of the medical team.
2. Doctor visits may not be in the office. The visit may be by phone or by secure web visits. Or it will be a group office visit for such things as routine diabetes management or for a routine blood pressure check-up.
3. Access to primary care will be 24 hours a day and 7 days a week. So when you are real sick at 10 PM on a Friday night, you talk to a provider by phone or by the web who has access to your electronic medical records and your doctor’s latest notes. He can either solve your problem or direct you to the best urgent care or emergency care facility for the problem you are having.
4. Depending on whether federal funding is available, we may see continued expansion of the federally qualified health centers, such as Westside here in Dover. The federal centers offer the ideal of a centralized point of delivery for, not only medical care, but also dental, psychiatric, psychological, social support services, and case management. Because of these additional services, their overhead costs per physician are many times greater than any private practice could possibly afford. This may be an example of the government taking the lead in redefining primary care, but it is being done with large government subsidies. No private practice could afford to provide this full array of services. Unfortunately, they don’t seem to be able to recruit and retain physicians any better than the private practices.
5. The trend nationally is toward large, merged physician groups. An example nearby is PMSI, a physician-owned multispecialty group practice with about 17 offices in Berks, Chester and Montgomery Counties in Southeastern Pennsylvania. Another example in neighboring Virginia is Riverside Health System which has over 300 physicians in the Hampton Roads area. A third example is Primary Care Health Partners of Vermont which is a large primary care medical group with offices throughout Vermont and upstate New York.
Electronic Medical Records (EMR)
Doctors are buying EMR systems for their offices. We are doing this because we want to and we know it is useful, but also because we are getting sizeable incentive bonuses from the federal government when we achieve certain benchmarks in the implementation of EMR. Plus we know our pay will be cut in the near future if we don’t have an EMR. EMR allows us to email prescriptions, track our performance, and identify deficiencies in your health care. It also allows the insurers, both the government and the private insurers, to track our performance and collect large amounts of data on the doctors and the patients. EMR is supposed to reduce errors, improve documentation, and reduce wasteful duplication of services such as lab work and x-rays. Plus, it gives you online access to your medical records.
Despite the incentive bonuses, EMR systems are very expensive to buy and maintain, especially for a small practice. The high cost of EMR is one reason why new primary care doctors do not want to go into private practice. Many small practices are already feeling the panic of a failed financial investment in EMR. Also, the EMR systems that are being sold today do not communicate with each other which becomes a barrier when doctors try to coordinate your care with other providers.
Private practice doctors or hospital employees
Can primary care medicine best be delivered by physician groups independent of the hospital or should primary care physicians/providers be employed by the hospital? Does a business association between doctor and hospital, especially if it is a for-profit hospital, create a conflict of interest? As employees of the hospital, do primary care physicians have an equal voice in the management of health care delivery or would there be financial incentives and constraints that prevent them from meeting their professional commitment to patients.
The attraction of the hospital is it has the financial resources to invest in and maintain an EMR system and to hire support staff such as nurse practitioners and health coaches. But if the doctors merge into very large private practices, they may be able to make these investments on their own. And I think that the doctors can better direct primary care if they are outside of the influence of the hospital’s financial concerns and the historic dominance of the specialists such as the cardiologists and the surgeons.
Our Challenge
The only way primary care providers will achieve the respect and attract the investments we need is to organize ourselves to deliver the care that matters to patients, to deliver that care at lower cost, and to provide value to employers and insurers. We must become creative at solving the problems of high quality and efficient care.
Here are some questions that I ask you to think about:
1. What are your experiences with primary care medicine?
2. Would you be willing to attend and pay for a “group visit” with say five other patients and a nurse practitioner to discuss your hypertension in place of a regular one-on-one visit with the doctor?
3. Would you be willing to pay to talk to your doctor on the phone for a “phone visit” to take the place of a regular office visit?
4. Would you be willing to pay to communicate with your doctor through a secure web site for a “web visit” to take the place of a regular office visit?
Source: delaware.newszap.com
Mental hospital refuses to be nursing care
 Hey Ma’am. Give us Rp 2,000 [20 US cents]” a woman called out as The Jakarta Post passed by her at Soeharto Heerdjan Mental Hospital. She sat with two other patients behind the bars separating the patient area from the public area.
Hey Ma’am. Give us Rp 2,000 [20 US cents]” a woman called out as The Jakarta Post passed by her at Soeharto Heerdjan Mental Hospital. She sat with two other patients behind the bars separating the patient area from the public area.
The patients wore T-shirts and trousers. Most were bald and thin. They looked at people passing in front of them with curiosity, or yelled in a strange manner.
Although several buildings are old, the hospital is quite clean — at least the area that visitors can access. The floor is shiny and janitors swab the tiles every time it looks dirty.
Few know what happens in treatment wards or isolation rooms, because only nurses and doctors are allowed to go there.
It is not easy for visitors like journalists to obtain access to the hospital. One has to meet with hospital authorities and sign an agreement with several stipulations, including a ban on taking close-up photos and mentioning the names of patients. The permit process takes hours.
This is the situation at the mental hospital in Grogol, West Jakarta, the biggest state mental hospital in Indonesia. The hospital accommodates 300 patients and serves 150 patients with mental disorders daily. There are 13 doctors, mostly psychiatrists, and 200 nurses.
Soeharto Heerdjan medical director Reza Syah told the Post the hospital treated patients with severe mental disorders like schizophrenia, bipolar disorder, acute hallucinations and severe depression.
Usually patients come from Jakarta and nearby municipalities like Tangerang, Depok and Bekasi. Some are beggars or homeless.
“Based on research, only 2.5 percent of severe mental disorder patients are treated in mental hospitals, but patients with light disorders or more than 90 percent are in the community,” Reza said.
He said there were many symptoms of mental disorders. People often forget that worry, stress, phobias, paranoia or senility can be symptoms, which many suffer from.
Today, Reza is trying to change the image of the mental hospital as a place offering nursing care for patients. Previously, families took patients to the hospital and left them there for years.
“We want to serve more patients so we hope after 21 days of intensive treatment they can go home and then we routinely check their health at the hospital,” Reza said.
But what happens if the family refuses to care for the patient?
“They can ask a social agency to take care of them. But here, in the hospital, we just treat them medically,” he said.
Reza believes medicine can be effective after two weeks of treatment.
“This strategy will help other patients who need medical treatment. Our capacity is small and many patients must get fair treatment as well,” he said.
However, Reza said many patients who were allowed to go home then forgot to consume their medicine. No wonder many have to be re-treated in the hospital later.
“The medicine is important. But we have to understand they don’t have money to buy medicine,” he said, adding that the majority of patients were poor.
Source: thejakartapost.com
Basuki Ingatkan Rumah Sakit tidak Bohong soal Obat
 Jakarta: Untuk mengantisipasi pembengkakan biaya obat-obatan yang dikeluarkan dan pemberian obat yang tepat kepada pasien,
Jakarta: Untuk mengantisipasi pembengkakan biaya obat-obatan yang dikeluarkan dan pemberian obat yang tepat kepada pasien,
Wakil Gubernur DKI Jakarta Basuki Tjahaja Purnama menginstruksikan Inspektorat Provinsi DKI Jakarta memeriksa kualitas dan kuantitas obat di Rumah Sakit Umum Daerah (RSUD) DKI.
“Saya sudah suruh inspektorat provinsi untuk periksa obat di RSUD milik Pemprov DKI Jakarta. Sebab ada kasus saat pegawai sakit, dokter kasih obat banyak. Ternyata tidak dipakai semuanya, lalu obatnya dibeli lagi dengan separuh harga,” kata Basuki di Jakarta, Sabtu (23/3).
Basuki mengaku memiliki pengalaman dalam dunia kesehatan, khususnya obat-obatan selama 13 tahun. Sebab, dulu ibunya mempunyai apotek dan sering menyuruhnya membeli obat-obatan di Pasar Pramuka, Glodok dan Pasar Pagi.
“Saya dilatih untuk mengepak barang dari pukul 04.00. Sejak SMA, selain sekolah, saya selalu beli obat dan peralatan kesehatan lainnya. Saya mengerti diskon dan expired obat seperti apa. Makanya jangan bohongi saya. Saya sudah suruh inspektorat untuk periksa obat di RSUD,” tegasnya.
Praktik penipuan obat-obatan merupakan salah satu masalah dalam pelayanan kesehatan di Jakarta. Harusnya, Jakarta bercermin pada India dan China yang berhasil meningkatkan kualitas pelayanan kesehatan. Selain memberikan obat-obatan murah, dokter pemerintah juga tidak boleh praktik di luar RS pemerintah daerah atau pusat.
“Yang penting bagi kami adalah gotong royong supaya Indonesia punya Badan Penyelenggara Jaminan Sosial (BPJS) tahun depan dan dilakukan di Jakarta sebagai proyek percontohan. Saya janji setelah sistem ini jalan dan dievaluasi untuk mengetahui kelemahannya di mana. Kami juga mau kasih hibah bagi rumah sakit yang mau perbanyak kelas III. Kita akan berikan tambahan koefisian luas bangunan. Rumah sakit yang mau bikin kampus pendidikan kedokteran, kami akan bantu,” ujarnya.
Dia menjelaskan penerapan sistem Indonesia Case Based Group (INA CBG) merupakan sistem yang buruk dari yang terburuk untuk rumah sakit. Karena itu, Basuki meminta pihak rumah sakit jangan memperdebatkan nilai yang akan didapatkan, namun yang terpenting sistem tagihannya dapat dibayar tepat waktu dan tidak memakan waktu terlalu lama.
“Setelah dua atau tiga bulan akan ada evaluasi. Nanti baru kita tahu biaya pokok dari rumah sakit berapa. Karena RSUD juga agak ngedumel masalah biaya, sebab rumah sakit kita juga banyak merekrut tenaga yang bukan dari PNS, sehingga mengeluarkan biaya besar,” ungkapnya.
Sumber: metrotvnews.com
Menjadikan puskesmas sebagai ujung tombak
 Sejak Kartu Jakarta Sehat (KJS) mulai diberlakukan November tahun lalu, pasien Rumah Sakit Umum Daerah (RSUD) milik Pemerintah Provinsi DKI Jakarta dan beberapa rumah sakit swasta ditunjuk membludak. Antrean panjang terjadi mulai dari loket antrean verifikasi data calon pasien, loket nomor urut, hingga antrean klinik dan poli. Bahkan di beberapa RSUD, antrean penanganan operasi dan rawat inap juga terjadi.
Sejak Kartu Jakarta Sehat (KJS) mulai diberlakukan November tahun lalu, pasien Rumah Sakit Umum Daerah (RSUD) milik Pemerintah Provinsi DKI Jakarta dan beberapa rumah sakit swasta ditunjuk membludak. Antrean panjang terjadi mulai dari loket antrean verifikasi data calon pasien, loket nomor urut, hingga antrean klinik dan poli. Bahkan di beberapa RSUD, antrean penanganan operasi dan rawat inap juga terjadi.
Misalnya di RSUD Pasar Rebo. Kepala Satuan Pelaksana Marketing dan Humas RSUD Dedy Suryadi mengatakan sejak KJS diberlakukan antrean pasien meningkat 50 persen. Bila sebelumnya antrean sebanyak 200 hingga 300 orang per hari, kini mencapai 500 orang saban hari. Padahal kamar rawat inap kelas tiga, khusus untuk pasien KJS jumlahnya terbatas. “Jadi antrean ya wajar, makanya sekarang diperbaiki. Kamar pasien kelas dua juga sudah diubah untuk pasien miskin,” kata dia ketika dihubungi merdeka.com, Kamis pekan lalu.
Merdeka.com sempat melongok bangsal cempaka untuk rawat inap pasien operasi bedah RSUD Pasar Rebo. Bangsal itu dibagi menjadi dua kelas: dua dan tiga, masing-masing mendapat jatah tiga kamar. Bangsal pasien kelas tiga, khusus pasien miskin sudah terisi penuh. Bangsal kelas dua untuk pasien umum tanpa KJS, rupanya masih menyisakan beberapa kamar kosong.
Padahal Gubernur DKI Jakarta Jokowi beberapa waktu lalu sempat meminta RSUD mengubah bangsal kelas dua menjadi kelas tiga. Seorang petugas keamanan kamar rawat inap pasien, sebut saja namanya Iqbal, mengatakan kondisi mirip juga terjadi di bangsal rawat inap poli penyakit lain. “Sama saja, mas. Kalau ada yang kososng, mungkin orangnya lagi operasi,” kata dia.
KJS untuk warga miskin pemilik identitas Jakarta. Jaminan kesehatan ini dilandaskan pada Undang-undang Nomor 40 Tahun 2004 tentang Sistem Jaminan Sosial Nasional. Pemerintah Jakarta menggandeng 95 rumah sakit, terdiri dari 22 rumah sakit milik pemerintah dan 73 rumah sakit swasta untuk melayani pasien KJS ini.
Namun setelah lima bulan berjalan, beberapa masalah muncul, salah satunya antrean perawatan itu. Antrean ini sebenarnya sudah diprediksi oleh pemerintah. Oleh sebab itu, kata Dedy, sekarang waktunya penataan. Bulan depan, dia melanjutkan, mekanisme pembayaran, termasuk verifikasi data pasien diperketat, ditangani langsung oleh PT ASKES.
Selain itu, data calon pasien pun ditelisik. Misalnya, apakah penerima KJS ini seluruh warga Jakarta atau tertentu, indikator warga penerima harus jelas, bisa mengacu kepada data masyarakat miskin dari Badan Pusat Statistik. Perbaikan lain menyangkut sarana: bangsal rawat inap, alat kesehatan, sumber daya manusia, termasuk kejelasan payung hukum.
Perbaikan juga harus menyentuh 89 puskesmas di seluruh Jakarta sebagai tempat pelayanan kesehatan pertama. Alat kesehatan puskesmas diperbaiki, pegawai dibangun, dan pendidikan kesehatan kepada masyarakat dilakukan sejak dini. Bila puskesmas bagus, masyarakat akan banyak berobat ke sana.
Bila pasien di puskesmas tidak tertangani, baru kemudian dirujuk ke RSUD. Kalau di RSUD tidak mampu, dirujuk ke Rumah Sakit Umum Pusat (RSUP) Nasional, misalnya RS Cipto Mangun Kusumo. “Tapi kalau pasien bisa ditangani di tingkat puskesmas, tidak perlu lagi ke rumah sakit, itu yang kami usulkan kepada gubernur,” kata dia.
Sumber: merdeka.com
Pengantar 25-30 Maret 2013
Memecahkan Kode Perubahan
 Semua sudah menyadari bahwa perubahan tidak dapat dihindari, namun dapat diantisipasi dan dikelola. Tulisan sebelumnya membahas mengenai delapan kesalahan terbesar yang terjadi selama proses transformasi yang menyebabkan mengapa proses transformasi gagal
Semua sudah menyadari bahwa perubahan tidak dapat dihindari, namun dapat diantisipasi dan dikelola. Tulisan sebelumnya membahas mengenai delapan kesalahan terbesar yang terjadi selama proses transformasi yang menyebabkan mengapa proses transformasi gagal
Salam hangat
Toronto General Hospital’s ‘operating room of the future’
Cancer surgeons will soon begin operating in high-tech $10-million suite, which features sophisticated scanning equipment to help guide instruments.
 O.R. Number 19 at the Toronto General Hospital is as fine a working surgical suite as you’re liable to find on Earth.
O.R. Number 19 at the Toronto General Hospital is as fine a working surgical suite as you’re liable to find on Earth.
A bit shopworn, jumbled and rank with disinfectants, sure. Yet it’s crammed with some of the most sophisticated gadgetry in the cutting trade today.
But Dr. Jonathan Irish — a childlike eagerness in his voice — is anxious to move next door.
“Wait until you see it,” the head of surgical oncology at the affiliated Princess Margaret Cancer Centre says as he heads down the hall. “Just wait.”
To the sucking sound caused by the positive pressure on the other side, Irish swings open the door to O.R. Number 20 and raises his hands with a “ta-dah” flourish.
“Welcome to the operating room of the future.”
The future of surgery that Irish reveals here appears to be bright. Gleaming even.
Indeed, futuristic is as apt a word as any to describe the suite — known as the GTx, for “guided therapeutics.” Surgeons will begin performing operations here in the coming weeks.
“This is big tech, big space . . . and certainly the cutting edge,” says Irish, as he launches a tour of the $10-million facility at the General’s University Ave. plant.
The first thing he points to is the obvious — the room’s size. At roughly 160 square metres, it is about three times larger than a standard operating room in most modern hospitals.
That space is far from a luxury, however. It’s needed to house the starship array of imaging equipment that whirs into motion around a central operating table.
These computed tomography (CT) scanners have been deployed to capture tumors and other surgical targets with unmatched precision — and to guide physicians to them via the safest and most optimal routes.
As such, the GTx, which will be used extensively for cancer surgeries, fits in well with Princess Margaret’s current $1-billion fundraising campaign.
One of the key goals of that effort is to fund and support research into the early detection of tumours, when they are at their smallest and most treatable stages.
However, while tiny tumours present optimal treatment targets, they also make for elusive ones.
“So the concept of using new technologies to target (things like tumours) in surgery is something that is a huge platform for our billion dollar challenge,” says Irish.
“The eyes of the future surgeon, the hands of the future surgeon, the knife of the future surgeon is all part of that package,” says Irish.
The room’s new CT tools can create, in real time, a GPS-like guidance system through the perilous interior of the human body.
Such aids will be invaluable to surgeons like Irish, who specializes in head and neck cancers.
Often using the nasal cavity as a point of attack, Irish must guide his tiny drills — mounted at the end of flexible tubes — through a fraught landscape, jammed up against brains and arteries and optic nerves.
But now it will be more than just his eyes in the room. “We can also use this technology to be our eyes,” he says.
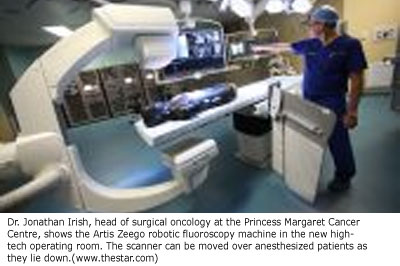
The first-line set of prying electronic eyes will be provided by the room’s Artis Zeego robotic fluoroscopy machine.
This impressive, C-shaped scanner — about 1.5 metres in diameter — is the newest generation of a device that was pioneered over the past decade by Toronto General and Princess Margaret researchers to peer inside bodies.
The machine — its C-ends capped with the actual CT scanning plates — can be moved over anesthetized patients as they lie on the operating table.
A hinged attachment to its base then allows the scanners to revolve around the patient and create a three-dimensional image of the surgical site as the operation progresses.
The machine, which had to be manoeuvred to the table manually during its previous, experimental usage, has offered a powerful tool for surgeons like Irish, who have long used other types of CT images to direct their instruments during operations.
The pictures they had available, however, were often days old, Irish says.
The major advance with the new GTx-based device is its robotic arm mount — similar to those used in auto assembly plants — which can easily and quickly move the scanner in and out as often as a surgeon desires.
“This gives us real time, on-the-table imaging, allowing us to update the (pictures) whenever we want,” he says.
“So we can get essentially GPS guidance with an image we’ve done seconds ago. And this is important, because during an operation, things can move. Things can change.”
Combined with some potent computer graphics programming, these fresh images can be presented in several ways as they flash up on two massive flat screens suspended above the operating table.
Most notable of these imaging options is one that will be uniquely available to GTx surgical teams.
In it, the nerves, vessels or brain bits that press in around the target tumours will be sheathed in computer-generated fencing — a virtual chain-link protection that keeps surgeons away from these critical tissues.
And as the tube-mounted scalpels — miniature drills or pulsing lasers — move in on the cancers, real-time imaging tracks their progress through this graphically protected anatomy, with the surgeon able to watch the motions on screen.
If any of these protected spaces are approached too closely, he says, an alarm will sound. If they are breached, the electronic scalpel will shut down.
“It creates no-fly zones to prevent collateral damage,” Irish says.
The thought of ceding such operational control to a computer might not sit well with many surgeons.
But Irish says most will simply accept such restrictions on their surgical autonomy as sensible and helpful advancements.
“This technology elevates an excellent surgeon to be able to do things that we weren’t able to do before,” he says. “I don’t see it as a challenge; I see it as a great opportunity.”
And, in the end, Irish says, surgeons can always turn the technology off if they want.
For even sharper images during operations, GTx surgeons will also have access to a more powerful CT machine, the nearby Siemens dual-energy CT Flash scanner to the table’s right.
This O-shaped scanner can plumb images at smaller resolutions and in deeper parts of the body than its robotic counterpart, Irish says.
Because of its size and weight, however, patients must move to the machine and be fed through its circular aperture.
This would be an immensely complex and disruptive undertaking in traditional operating rooms, with much of the surgical team being required to physically hoist the table, patient and attendant wires and tubing over to the scanner.
But in the new room, this entire operation is performed automatically, with the table swinging over and being fed through the scanner at the press of a button.
The amped-up and automated imaging systems provided by the room’s scanner tandem will become increasingly important at the hospital, as research to detect smaller and smaller tumours bears fruit.
“Let’s say we now can detect a very, very small lung cancer . . . often the standard of care is to repeat a CT scan in a few months to see if it’s grown,” Irish says.
But with the GTx’s real-time guidance capacity, surgeons can go in right away with an increased confidence of finding and removing the cancer, he says.
Its advanced equipment and plush space, however, will not be the only things that separate the GTx from other operating rooms.
Its signature feature will be its role as the world’s first research-based operating room, Irish says.
Patients wheeled into O.R. Number 20 will automatically enter medical trials — research projects meant to compare its surgical procedures and equipment with those used in standard operating facilities.
“It’s a research operating room; you can’t actually be a patient in this operating room unless you’re part of a research trial,” Irish says.
“The other 19 operating rooms are for the everyday stuff. This operating room is for the use of innovative technologies.”
Surgery has traditionally been a discipline apart from other branches of medicine, where rigorous, randomized trials of new medications and procedures must prove out their worth and value scientifically over older treatments.
“But the concept of developing (surgical) technologies . . . was ‘this is interesting, let’s just try it,’ ” Irish says.
After trials in animal models and cadavers, surgical procedures and equipment were brought into clinical settings, but were not necessarily matched systematically against older techniques and technologies to prove their superiority.
Irish says the GTx will change that.
“The first in-human technologies will be used here . . . and evaluated here,” Irish says.
The success of the new equipment and techniques deployed in the room — now and in the future — will be evaluated based on comparisons with the outcomes of surgeries preformed by the same physicians in the hospital’s older suites.
The high-tech cutting room will also be used to evaluate some purely human factors, such as alternative nursing roles and new concepts in surgical team configurations.
But because most of the research projects will be testing new scanners, guidance systems and the like, engineers and physicists will often join the standard roster of surgeons, nurses and anesthetists around its operating table.
Irish points, for example, to Michael Daly, whose role as a biomedical engineer would have typically seen him toil exclusively in laboratories, helping to create improved scanning and radiation devices.
“In our new O.R. of the future . . . an engineer like Michael, will be right in there to help design new technologies to develop the new eyes of the surgeon, or hands of the surgeon or new knife,” Irish says.
For Daly, the idea that his career would take him into an active O.R. never crossed his mind.
“I did applied math and electrical engineering (at school), but I spend many days . . . in the operating room, seeing the clinical challenges and learning about anatomy,” he says.
“So I get a better idea of what technology is feasible and what can be effective.”
Source: thestar.com
Deadly bacteria hitting Louisville hospitals, long-term care facilities
 They’ve been called “nightmare bacteria” — deadly superbugs known as CRE that strike hospitalized patients and kill as many as half who get bloodstream infections.
They’ve been called “nightmare bacteria” — deadly superbugs known as CRE that strike hospitalized patients and kill as many as half who get bloodstream infections.
And they’re on the rise — in Louisville and across the nation.
The U.S. Centers for Disease Control and Prevention issued a strong warning this month, saying “action is needed now to stop these deadly infections” that have been treated in nearly 200 U.S. hospitals during the first half of 2012.
While neither Kentucky nor the federal government tracks individual cases, local hospitals officials say they’ve seen a growing number in recent years — and they’re enacting measures to combat CRE — short for carbapenem-resistant Enterobacteriaceae, a family of germs that has high resistance to antibiotics.
“If it gets in the community and spreads, we’re in trouble,” said Dr. Kevin Kavanagh, who leads the Somerset, Ky.-based watchdog group Health Watch USA.
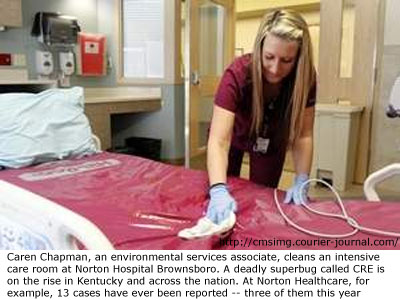
University Hospital officials said they had a case this year in which the patient died, and Norton Healthcare says three of its 13 cases since 2010 have occurred this year, prompting Chief of Microbiology Alan Junkins to say, “I’m kind of worried it’s getting worse.”
“In my mind, this is one of the most worrisome (group of) germs we as a society have to deal with,” said Dr. Paul Schulz, Norton system epidemiologist. “You really get this combination of potentially high virulence and very difficult resistance” to antibiotics.
Experts say the problem is fueled by the overuse of antibiotics and gaps in infection control in hospitals and long-term care facilities — the same problems that give rise to other pernicious, health-care-associated infections such as MRSA and C. difficile (commonly called C. diff).
Officials at Norton and other facilities say they are taking steps to prevent infections — stressing measures such as hand-washing, room-cleaning and using antibiotics more wisely.
The Kentucky Department for Public Health, meanwhile, educates health care providers about preventing superbugs and will soon tap into CDC statistics on health-care-associated infections.
Source: courier-journal.com
Ini Dia Kode Gawat Darurat di RSCM
 JAKARTA–Rumah Sakit RS Cipto Mangunkusumo, memiliki kode percakapan khusus apabila terjadi situasi gawat darurat.
JAKARTA–Rumah Sakit RS Cipto Mangunkusumo, memiliki kode percakapan khusus apabila terjadi situasi gawat darurat.
Keadaan yang dimaksud gawat itu seperti kebakaran, ancaman bom, perampokan, penyanderaan, serta kondisi lainnya.
Berdasarkan keterangan para pegawai rumah sakit, kode-kode agar membuat pasien tidak panik saat proses evakuasi.
Kode-kode ini adalah kode percakapan antar pegawai rumah sakit ketika terjadi kondisi gawat.
“Kan tidak mungkin, ketika terjadi kebakaran atau ada penyanderaan lalu pegawai lekas memberitahukan begitu saja kepada pasien. Bisa lari sendiri-sendiri nanti pasiennya,” ujar salah satu pegawai kepada wartakotalive.com.
Salah satu percakapan khusus itu, yakni ‘code red’ apabila terjadi kebakaran di area rumah sakit.
Kemudian, keadaan gawat lainnya juga disebut dengan ‘code’ di depannya, lalu kata belakangnya kembali mengambil nama warna dalam bahasa Inggris.
Setiap kondisi gawat ditunjukkan dengan nama warna dalam bahasa Inggris.
Sumber: jakarta.tribunnews.com
Pengamat: Keberadaan RSUD Banten Akan Munculkan Persoalan Baru
 Serang – Keberadaan Rumah Sakit Umum Daerah (RSUD) Banten sebagai rumah sakit rujukan dinilai akan memunculkan masalah baru. RSUD yang ada dipastikan tidak akan efisien dan efektif. Persoalan baru yang dihadapi yakni terkait belanja operasional dan managerial yang tidak terkait dengan pelayanan langsung.
Serang – Keberadaan Rumah Sakit Umum Daerah (RSUD) Banten sebagai rumah sakit rujukan dinilai akan memunculkan masalah baru. RSUD yang ada dipastikan tidak akan efisien dan efektif. Persoalan baru yang dihadapi yakni terkait belanja operasional dan managerial yang tidak terkait dengan pelayanan langsung.
Pengamat Ekonomi dari Universitas Sultan Ageng Tirtayasa (Untirta) Banten Dahnil Anzar, menegaskan seharusnya Pemprov Banten membantu mengoptimalkan pelayanan RSUD kabupaten/kota yang sudah ada.
“RSUD yang didirikan Pemprov Banten justru akan memunculkan masalah birokrasi baru,terutama berkaitan dengan belanja operasional. Padahal, sejumlah kabupaten/kota yang ada di Banten, masing-masin sudah memiliki RSUD. Seharusnya Pemprov Banten membantu mengoptimalkan pelayanan RSUD yang ada di kabupaten/kota seperti RSUD Serang, Pandeglang, Lebak dan Tangerang, dengan bantuan pendanaan dari Pemprov Banten,” tegas Dahnil di Serang.
Menurut Dahnil, Pemprov Banten seharusnya fokus pada tugas perbantuan memberikan asistensi, koordinasi pembangunan dan pelayanan dasar, mendorong stimulus seperti infrastruktur dan lain-lain.
“Pembangunan RSUD Banten tidak sesuai dengan tugas pokok pemprov. Seharusnya pemprov memberikan asistensi pendanaan supaya RSUD yang ada di kabupaten dan kota se-Banten dapat meningkatkan pelayanan dan kualitasnya,” katanya.
Sebelumnya, Wakil Gubernur Banten Rano Karno menjelaskan keberadaan RSUD Banten merupakan solusi terhadap persoalan pasien yang tidak mampu yang tidak tertampung di RSUD kabupaten/kota yang ada selama ini.
“Berdasarkan hasil identifikasi yang dilakukan Pemprov Banten pada RSUD yang ada di kabupaten/kota, menunjukkan adanya pasien yang tidak mampu yang sebagian tidak tertampung. Selain itu, masih tingginya angka kematian ibu dan bayi dan tingginya rujukan pasien ke luar provinsi menjadi alasan dan dasar dibangunnya RSUD Banten. Karena itu, dengan beroperasinya RSUD Banten maka kebutuhan masyarakat terhadap akses pelayanan kesehatan bisa semakin dekat, mudah dan terjangkau,” ujar Rano.
Rano Karno menjelaskan sebagaimana diatur pada pasal 10 Peraturan Menteri Kesehatan Nomor 340 Tahun 2010 tentang Klasifikasi Rumah Sakit, ditegaskan bahwa rumah sakit kelas B adalah rumah sakit yang memberikan pelayanan spesialis minimal delapan belas pelayanan dan sub spesialis. Selain itu, jumlah tempat tidur minimal 200 unit.
“Guna memenuhi tuntutan tersebut, di RSUD Banten telah disiapkan 184 tempat tidur dan pada tahun 2014 akan ditambah menjadi 216 tempat tidur. Ruang perwatan dan ruang penunjang lainnya juga akan ditambah,” jelasnya.
Sumber: beritasatu.com








