 Infections picked up in hospitals, nursing homes and doctor’s offices affect more than 1 million patients and are linked to nearly 100,000 deaths a year.
Infections picked up in hospitals, nursing homes and doctor’s offices affect more than 1 million patients and are linked to nearly 100,000 deaths a year.
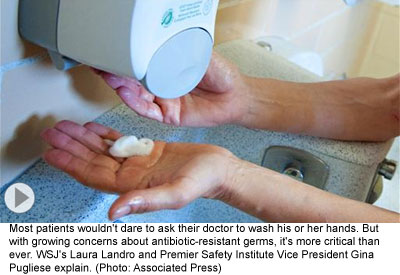
It’s a simple enough request, but for patients and families who feel vulnerable, scared or uncomfortable in a hospital room, the subject can be too intimidating to even bring up with a doctor or nurse: Have you washed your hands?
Hospitals are encouraging patients to be more assertive, amid growing concern about infections that are resistant to antibiotics.
Strict hand hygiene measures are the gold standard for reducing infections associated with health care. Acquired primarily in hospitals but also in nursing homes, outpatient surgery centers and even doctor’s offices, they affect more than one million patients and are linked to nearly 100,000 deaths a year, according to the Centers for Disease Control and Prevention.
Yet despite years of efforts to educate both clinicians and patients, studies show hospital staff on average comply with hand-washing protocols, including cleansing with soap and water or alcohol-based gels, only about 50% of the time. Two new studies show patients aren’t much more comfortable today than a decade ago with the idea of asking doctors and medical staff to lather up.
Hospitals have reduced certain infections over the past four years with measures such as removing unnecessary catheters and washing a patient’s skin before surgery with antibacterial soap. Some have lifted hygiene compliance to nearly 100% with strict “wash in, wash out” protocols, and some have designated unidentified staffers to secretly monitor co-workers. Some hospitals link merit increases to compliance and temporarily suspend clinical privileges of doctors who ignore the rules, says Gina Pugliese, vice president of the Safety Institute at hospital purchasing alliance Premier Inc. According to a 2010 study, a disciplinary program at the University of Kentucky Medical Center in Lexington that included suspending doctors’ privileges led to improved compliance rates.
More hospitals have turned to electronic sensors, thermal imaging and video cameras to monitor hand hygiene, and some are issuing badges that wirelessly record staffers’ use of hand hygiene stations before entering a patient room. Some monitoring systems emphasize patient engagement and sound an electronic alert to remind patients to speak up when a staffer enters the room.
The CDC has provided 16,000 copies of a video, titled “Hand Hygiene Saves Lives,” to be shown to patients at admission. In one scenario, a doctor comes into a room and the patient’s wife says, “Doctor, I’m embarrassed to even ask you this, but would you mind cleansing your hands before you begin?” The doctor replies, “Oh, I washed them right before I came in the room.” The wife says, “If you wouldn’t mind, I’d like you to do it again, in front of me.”
After patients at 17 hospitals run by Cincinnati-based Catholic Health Partners watched the video, there was a rise in both the proportion of patients asking staffers to wash their hands, and physicians and nurses reporting that they were asked, according to a 2010 study. “Hand hygiene is probably the most important thing health-care workers can do to protect their patients from infection,” says John Jernigan, director of the CDC’s hospital infection-prevention efforts who appears in the video. When patients speak up, it helps create “a culture of safety,” he says.
The nonprofit Association for Professionals in Infection Control and Epidemiology is kicking off a campaign this month including posters mailed to 15,000 hospitals with tips on how patients can take an active role. It suggests asking staff about hand hygiene and requesting that hospital rooms be cleaned if they appear dirty.
“We’ve been focusing on intensive interventions to improve hand hygiene among health-care workers for decades, yet we’ve really shown very little progress,” says Carol McLay, a Lexington, Ky., infection prevention consultant and chair of the committee that designed the campaign. “We are trying to empower patients and families to speak up and understand their role.”
At some hospitals, posters, bedside placards and buttons for staffers say, “Ask me if I’ve washed my hands.” Susan Coffin, a pediatric infectious disease physician at the Children’s Hospital of Philadelphia, says while many efforts are made in good faith, they are “insufficient to overcome some of these barriers.” She is co-author of a study, published in June in the American Journal of Infection Control, which found that 84% of parents were aware of infection risk yet only 67% would remind a health-care worker to wash their hands, most often because of concern about appearing rude or undermining authority. Yet 92% of parents said if a health-care worker invited reminders, they would be more likely to do so. The hospital is “trying to make it a more active conversation,” Dr. Coffin says. Admission packets offer detailed information on hand hygiene and nurses tell families that staffers welcome questions about hand washing.
In a study published in September in the journal Infection Control and Hospital Epidemiology, one-third of patients surveyed at the University of Pittsburgh Medical Center said they observed doctors failing to wash their hands, but nearly two-thirds said nothing to their doctor about hand hygiene. Most didn’t believe it was their role to do so and said they felt embarrassed or awkward and worried about reprisal.
Patients are more likely to ask nurses about hand hygiene, says Gregory Bump, associate professor of medicine. “There is something about the white-coat barrier that makes them reluctant to challenge doctors.” Physicians may resist assertive patients and seem unreceptive or even hostile to a question about hand washing, he says.
Patients, instead of receiving information about infections and hand washing, would prefer having staffers wear a button or light to indicate whether his or her hands had been washed, the study also found. UPMC is developing a system to measure and track hand-washing compliance, as well as computerized verbal reminders to patients to ask the employee to clean their hands when they enter the room.
Michael Gettes, 50, has been hospitalized several times and says he has never had to remind Dr. Bump, his primary physician, to wash his hands. He has asked other hospital staffers to do so. One doctor reacted negatively. “It put our relationship on a bad footing,” Mr. Gettes says. “Yes, you run the risk of upsetting someone who has been taking care of you. But it is my life. If they make a mistake I am impacted or I die.”
Gail Ulager, a 72-year-old kidney transplant recipient at UPMC, says she worries about the possibility of infection because she is taking drugs that suppress her immune system to prevent rejection of her new organ. She found a way to give the message to doctors, nurses and even her dentist without seeming disrespectful. “I always tell them that the transplant center insists that everyone washes their hands” she says.
Source: online.wsj.com








